Sedation and Anesthesia in Dental Treatments: Your Guide to Comfortable and Anxiety-Free Dentistry
Dental sedation and anesthesia are tools clinicians use to manage pain and anxiety, enabling safe and comfortable dental care for a wide range of patients. This guide explains how sedation (a spectrum of consciousness levels) and anesthesia (local or general loss of sensation or consciousness) work, why they matter for patients with dental anxiety or complex procedures, and how choices are made based on procedure type and medical history. Many patients avoid needed care because of fear or intolerance of procedures; understanding available options reduces that barrier and improves outcomes. In the sections that follow you will find clear definitions and a comparison of sedation versus anesthesia, an overview of the main types used in dental practice, guidance on who is a candidate, benefits and safety protocols, and practical preparation and aftercare checklists. Throughout we use current research perspectives (2022–2024), clinical best practices, and helpful decision aids so you can discuss options confidently with your dental team and prepare for any necessary appointments.
What Is the Difference Between Dental Sedation and Anesthesia?
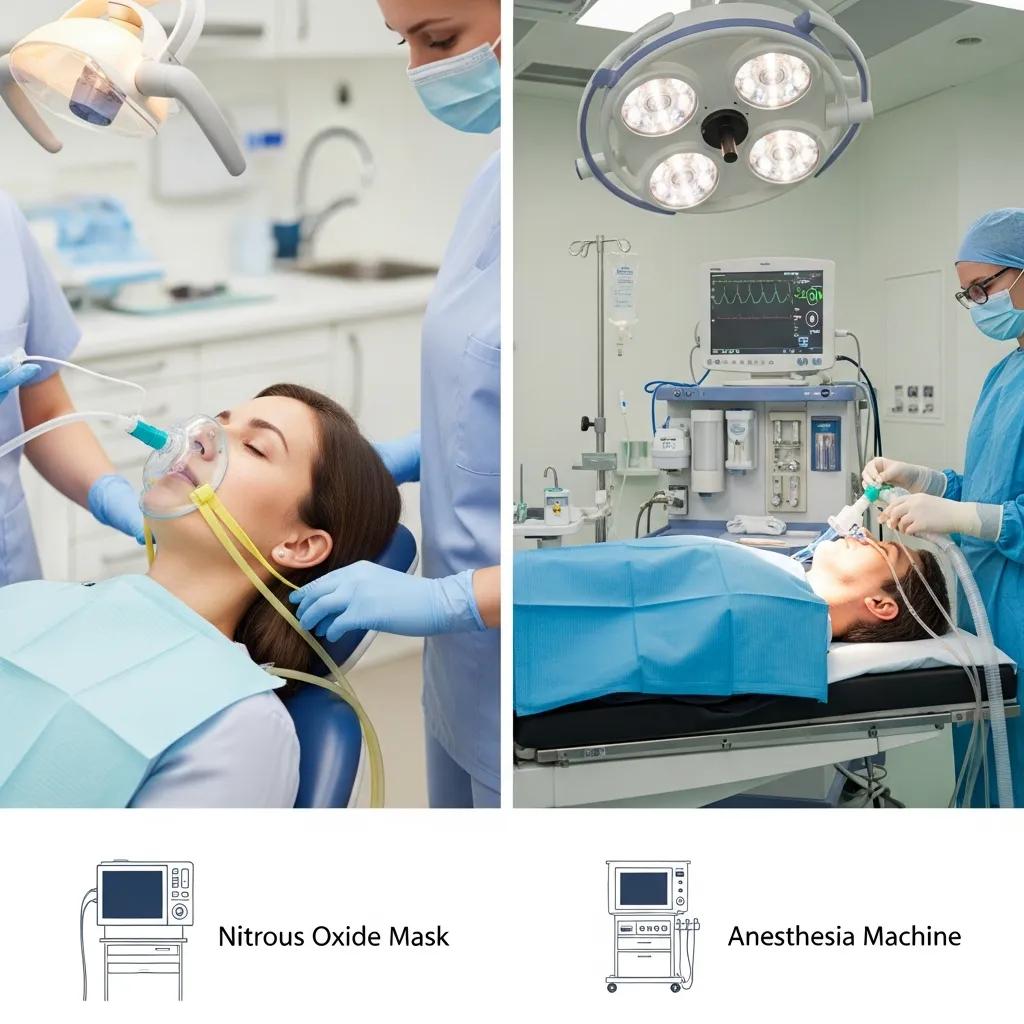
Dental sedation and anesthesia both control discomfort, but they differ in depth of consciousness and primary purpose. Sedation reduces anxiety and can range from minimal relaxation to deep sedation where responsiveness is reduced; anesthesia specifically blocks sensation at the local site or induces unconsciousness with general anesthesia for surgical procedures. Sedation is typically used to manage anxiety and improve tolerance during dental care, while anesthesia is chosen to eliminate pain during invasive or extensive surgery. Understanding these distinctions helps patients and clinicians match the technique to the procedure and patient health status. The next subsection explains how sedation specifically reduces anxiety and pain and improves the patient experience.
How Does Sedation Dentistry Help Manage Dental Anxiety and Pain?
Sedation dentistry reduces anxiety primarily by depressing central nervous system activity with medications such as benzodiazepines or inhaled agents, producing relaxation and decreased perception of time and discomfort. This mechanism decreases sympathetic arousal, which in turn lowers gag reflex, muscle tension, and procedural distress, making procedures more tolerable for anxious adults and children. For many patients, sedation enables completion of longer or multiple treatments in one visit, improving clinical efficiency and reducing repeat appointments. Monitoring during sedation—pulse oximetry, blood pressure, and trained staff—ensures safety while providing comfort. Understanding these effects sets the stage for when deeper interventions like intravenous moderate sedation become appropriate.
When Is Intravenous Moderate Sedation Used in Dental Procedures?
Intravenous (IV) moderate sedation is used to achieve a controlled state of relaxation and reduced anxiety while maintaining patient responsiveness and protective reflexes. It is particularly beneficial for patients with moderate to severe dental anxiety, those undergoing longer or more complex procedures, or when oral sedation is insufficient. IV sedation allows clinicians to titrate sedative agents such as propofol, midazolam, and fentanyl in real time to maintain the desired sedation depth. Continuous monitoring of vital signs including pulse oximetry, blood pressure, and cardiac rhythm ensures patient safety. Recovery from IV sedation is typically faster and smoother than deeper anesthesia, with patients regaining full alertness under supervision before discharge. This approach balances comfort, safety, and procedural efficiency for many dental treatments.
Attract new patients and retain existing ones by providing comprehensive information, building trust, and facilitating appointment bookings.
What Are the Main Types of Dental Sedation and Anesthesia?
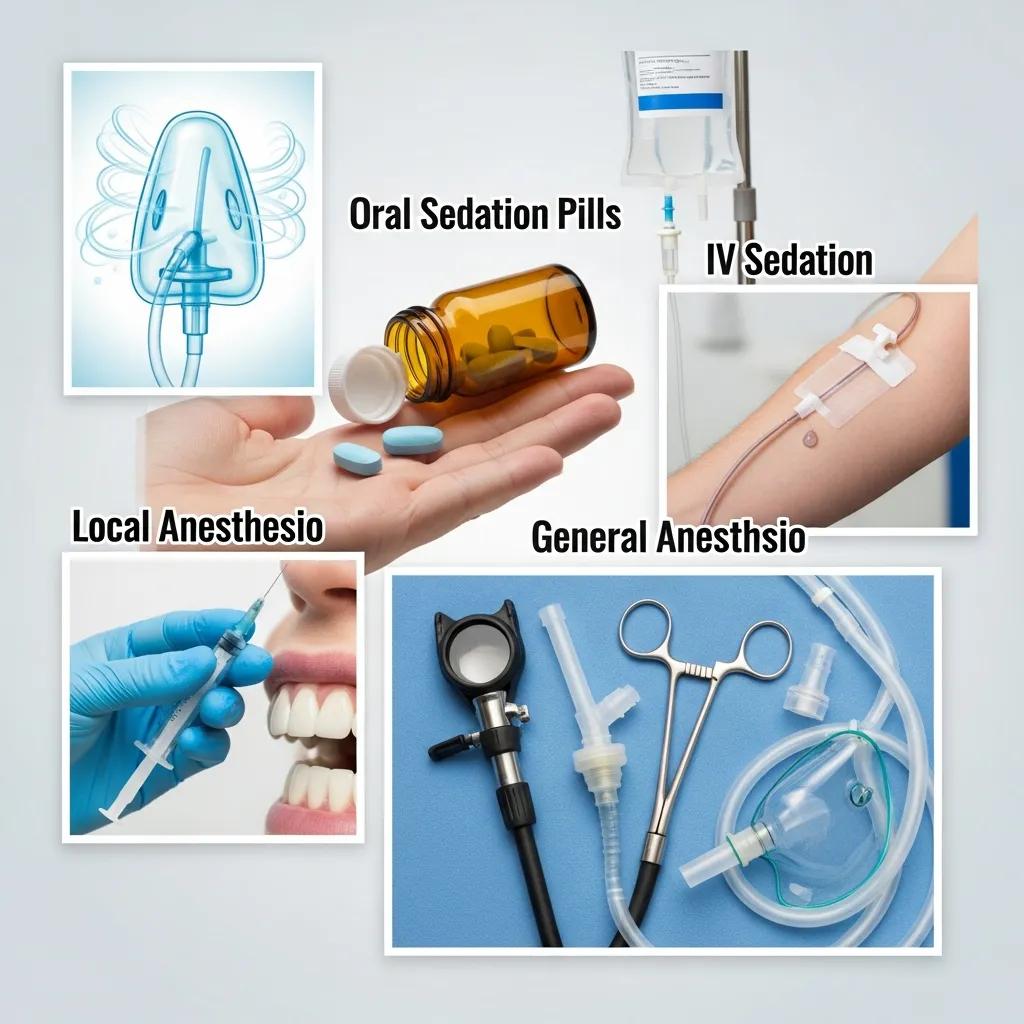
There are five principal approaches used in dental practice: nitrous oxide (minimal sedation), oral conscious sedation (pills), IV sedation (moderate sedation), general anesthesia (complete unconsciousness), and local anesthesia (site-specific numbing). Each method differs by administration route, onset and duration of effect, monitoring requirements, and typical clinical uses, so clinicians select the modality that balances patient safety, comfort, and procedural needs. Knowing the practical differences helps patients ask informed questions about medications, fasting, and escort requirements. The following subsections describe each type, starting with the commonly used nitrous oxide.
How Does Nitrous Oxide Sedation Work for Relaxed Dental Procedures?
Nitrous oxide, often called laughing gas, is inhaled through a mask and produces rapid-onset minimal sedation that reduces anxiety while preserving patient responsiveness and protective reflexes. This inhalation agent works by modulating central nervous system pathways to create relaxation and mild analgesia; effects begin within minutes and dissipate quickly once administration stops, allowing most patients to leave without a prolonged recovery period. Nitrous oxide is well-suited for short procedures, pediatric patients with mild anxiety, and adults who prefer a reversible, titratable option. Because recovery is fast, monitoring is brief, and the agent can be easily adjusted, nitrous oxide is often the first-line sedation for minimal anxiety management. The next subsection explains oral sedation pills and their considerations.
What Should You Know About Oral Sedation Dentistry and Its Medications?
Oral sedation uses systemic medications—commonly benzodiazepines such as midazolam or diazepam—to produce moderate sedation that decreases anxiety and produces amnesia for the procedure, with effects that begin within 30–90 minutes and last several hours. Patients should expect slower onset, a need for fasting in some cases, and strict transport requirements so they avoid driving after the appointment; an escort is typically required to ensure safety after discharge. Oral sedatives interact with other central nervous system depressants and certain medical conditions, so a complete medication and health history is essential during pre-procedure screening. Discussing dosing, expected sedation level, and timing with your dental team helps avoid complications and ensures appropriate monitoring during the appointment.
How Is IV Sedation Administered for Deep Relaxation During Dental Work?
IV sedation delivers sedative agents directly into the bloodstream, allowing clinicians to titrate depth of sedation in real time and achieve moderate sedation depending on procedural needs and patient response; agents such as propofol, midazolam, and fentanyl are commonly used in controlled settings. IV access is established, medications are administered incrementally, and continuous monitoring—pulse oximetry, blood pressure, and cardiac rhythm as indicated—ensures patient safety while maintaining airway and ventilation as appropriate to the sedation depth. IV sedation is advantageous for long procedures or patients with high anxiety who require rapid adjustments in sedative depth and for whom oral options are insufficient. Clear pre-procedure instructions and an escort for post-op transport are essential parts of IV sedation planning.
Research indicates that intravenous sedation is a highly effective method for managing dental anxiety, though it necessitates advanced training beyond undergraduate education.
Intravenous Sedation for Dental Anxiety Management
Anxiety and phobia in dental procedures are common deterrents for patients visiting the dental care unit. For these individuals, procedural sedation may aid in completion of dental treatments. In most cases, the patients are conscious during sedation, thereby allowing spontaneous ventilation. Intravenous sedation (IVS) is widely used during dental treatment to relieve patient anxiety. IVS is the most effective route of administration to achieve this goal, but it requires advanced training, more than that provided during undergraduate education.
Current trends in intravenous sedative drugs for dental procedures, JY Yoon, 2016
What Are the Benefits and Uses of Local Anesthesia in Dentistry?
Local anesthesia—agents like lidocaine or articaine—blocks nerve conduction at the site of treatment to eliminate pain while the patient remains conscious, and it is the foundation of pain control in most dental procedures. Local anesthetics are rapidly effective, can be combined with sedation for both comfort and analgesia, and generally have predictable onset and duration that clinicians tailor to the procedure. Allergic reactions are rare but must be screened for, and clinicians select agents and techniques to minimize systemic absorption and toxicity. Combining local anesthesia with appropriate sedation often produces the best balance of safety, pain control, and patient cooperation for many restorative, endodontic, and surgical treatments.
Different sedation and anesthesia types vary by route, onset, duration, monitoring, and typical side effects. The table below summarizes these characteristics for quick comparison.
Different sedation and anesthesia methods have distinct monitoring needs and recovery expectations.
| Method | How It’s Given | Typical Onset & Duration | Monitoring Required |
|---|---|---|---|
| Nitrous Oxide | Inhalation via mask | Onset: minutes; Duration: minutes | Basic monitoring (pulse ox, vitals) |
| Oral Sedation | Oral tablets or capsules | Onset: 30–90 minutes; Duration: hours | Moderate monitoring; escort required |
| IV Sedation | Intravenous titration | Onset: immediate; Duration: procedure-dependent | Continuous monitoring (pulse ox, BP, possible EKG) |
| General Anesthesia | IV or inhalation in OR setting | Onset: rapid; Duration: controlled | Full anesthesia monitoring (airway, EKG, capnography) |
| Local Anesthesia | Injection at site | Onset: minutes; Duration: 1–6+ hours | Minimal monitoring; observe for allergies |
This comparison clarifies how route and monitoring affect choice of method and recovery planning.
Who Is a Candidate for Sedation or Anesthesia in Dental Treatments?
Candidates for sedation or anesthesia are identified by a combination of medical history, procedure complexity, behavioral factors, and age-related considerations. Medical conditions such as severe anxiety or phobia, certain cardiovascular or neurologic issues, and complex surgical needs can make sedation or general anesthesia appropriate; conversely, conditions that increase anesthetic risk require tailored planning and consultation. Behavioral indicators—uncontrolled gag reflex, inability to cooperate, or developmental disabilities—also influence candidacy for sedation approaches. The following subsections list common condition-procedure pairings and pediatric/special-needs considerations to guide decision-making.
Which Medical Conditions and Dental Procedures Require Sedation?
Certain procedures—like multiple dental implants, impacted wisdom tooth removal, and extensive bone grafting—often require sedation or anesthesia due to duration and invasiveness, while medical conditions such as severe dental anxiety, uncontrolled movement disorders, or conditions that complicate local anesthesia responsiveness may also indicate sedation. Clinicians weigh factors like airway risk, ASA classification, medication interactions, and the need for immobility when recommending a sedation level. A thorough preoperative evaluation includes medication reconciliation, review of cardiovascular and respiratory history, and discussion of fasting and escort plans to reduce perioperative risk. Matching the procedure and medical profile to the appropriate sedation modality ensures safety and effective pain control.
How Does Sedation Dentistry Support Children and Special Needs Patients?
For pediatric patients and individuals with developmental or behavioral challenges, sedation or general anesthesia can enable necessary dental care that would otherwise be impossible due to fear, limited cooperation, or medical comorbidities. Pediatric sedation protocols follow age-appropriate dosing, parental consent, and close monitoring with adherence to pediatric guidelines from professional organizations; sedation in these populations often emphasizes rapid recovery and airway protection. Caregivers receive detailed pre-visit instructions and post-operative monitoring plans to ensure safety at home after discharge. Specialized training and experience in pediatric and special-needs dentistry improve outcomes and reduce perioperative stress for both patients and families.
What Are the Benefits and Safety Considerations of Sedation Dentistry?
Sedation dentistry offers tangible benefits: reduced anxiety, improved procedural tolerance, ability to complete multiple treatments in one visit, and enhanced patient satisfaction and clinical efficiency. These benefits must be balanced with safety protocols—patient screening, informed consent, continuous monitoring, and staff trained in airway management—to minimize risk and ensure prompt response to adverse events. Transparent discussions about potential side effects (drowsiness, nausea), rare complications, and emergency preparedness build trust and help patients make informed choices. The next subsections outline practical patient-centered benefits followed by the specific safety systems that minimize risk during sedation.
How Does Sedation Improve Patient Comfort and Treatment Efficiency?
Sedation can transform the patient experience by reducing fear, preventing traumatic memories, and enabling complex or multiple procedures to be completed with less stress and fewer appointments; this often leads to faster treatment completion and better long-term oral health outcomes. For clinicians, improved patient cooperation reduces chair-time disruptions and allows for more predictable workflows and efficiency gains, such as restoring multiple teeth or performing surgical procedures in a single session. Examples include combining restorations and extractions under sedation to minimize total visits or using moderate sedation to facilitate lengthy endodontic or surgical work. Highlighting these practical benefits helps patients and clinicians choose the appropriate care pathway.
What Safety Protocols Ensure Risk Minimization During Sedation?
Safety during sedation relies on comprehensive pre-operative screening, informed consent, appropriate fasting guidelines, and monitoring standards—including pulse oximetry, blood pressure, and, when indicated, EKG and capnography—alongside staff trained in airway management and emergency protocols. Professional guidelines from organizations such as the American Dental Association (ADA) and the American Society of Anesthesiologists (ASA) recommend documentation of medical history, medication reconciliation, and clear discharge criteria; facilities should maintain emergency equipment and drug kits to manage rare adverse events. Continuous monitoring during and after sedation, plus a defined recovery observation period before discharge, ensures that any complications are detected and managed promptly. These protocols form the backbone of safe sedation practice and patient reassurance.
The consensus among experts is that light sedation for low-risk patients (ASA I and possibly II) is the safest approach in a dental outpatient setting.
Sedation Techniques and Safety in Dental Outpatient Settings
Sedation in dentistry is a controversial topic given the variety of opinions regarding its safe practice. This article evaluates the various techniques used to administer sedation in dentistry and specific methods practiced to form a recommendation for clinicians. Most of the literature revealed a consensus that light sedation on low-risk American Society of Anesthesiologists (ASA) groups, that is ASA I, and possibly II, is the safest method for sedation in a dental outpatient setting.
Techniques to administer oral, inhalational, and IV sedation in dentistry, 2016
Attract new patients and retain existing ones by providing comprehensive information, building trust, and facilitating appointment bookings.
- Reduced Anxiety: Sedation lowers fear and physiological stress during dental procedures.
- Improved Procedure Tolerance: Patients tolerate longer or more invasive treatments.
- Efficiency Gains: Multiple procedures can be completed in fewer visits.
- Safety Measures: Pre-op screening, monitoring, and trained staff minimize risk.
How Dental Sedation and Anesthesia Ensure Anxiety-Free Dental Care
Preparation and aftercare are essential components of safe sedation: clear pre-appointment fasting rules, medication guidance, and escort arrangements reduce perioperative risks, while structured post-sedation care ensures recovery and early identification of complications. Type-specific checklists help patients meet requirements for nitrous oxide, oral, IV, and general anesthesia and clarify what to expect immediately after treatment. The following subsections provide concise pre-appointment instructions by sedation type and a timeline for post-sedation recovery and warning signs that require prompt contact with the dental team.
What Are the Pre-Appointment Instructions for Different Sedation Types?
Pre-appointment instructions vary by modality but commonly include fasting for a specified time before IV or general anesthesia, withholding certain medications or adjusting doses after clinician review, and arranging a responsible adult to escort the patient home when sedation affects alertness. For nitrous oxide, light meals are often allowed and recovery is rapid; for oral and IV sedation, patients should avoid driving and plan for 24-hour reduced activity. Accurate medication lists and disclosure of alcohol, recreational drug use, and sleep apnea history are essential to prevent interactions and airway complications. Clear logistics and expectations reduce day-of-procedure anxiety and help clinicians provide safe care.
Pre-appointment EAV table below provides concise, type-specific checklists.
| Sedation Type | Pre-Appointment Instructions | Key Safety Considerations |
|---|---|---|
| Nitrous Oxide | Eat light meal unless instructed; inform clinician of recent cold/allergies | Rapid recovery; minimal fasting required |
| Oral Sedation | Follow fasting if instructed; bring medication list; arrange escort | Interaction with other sedatives; escort required |
| IV Sedation | NPO as directed; review meds; arrange transport | Airway monitoring; continuous vitals monitoring |
| General Anesthesia | Strict fasting; pre-op medical clearance as indicated | Requires anesthesiologist-level monitoring |
| Local Anesthesia | No special fasting generally; disclose allergies | Allergy screening; local toxicity precautions |
This table condenses pre-visit steps to help patients prepare appropriately for each modality.
What Post-Sedation Care Is Recommended for a Safe Recovery?
Post-sedation care emphasizes observation until stable, gradual resumption of fluids and light foods, avoidance of driving or operating machinery for the specified period, and clear instructions about medications and signs of complications such as prolonged vomiting, difficulty breathing, or uncontrolled bleeding. Recovery timelines vary: nitrous oxide recovery is rapid and patients often resume normal activities quickly, while oral and IV sedation may require several hours of supervision and restriction on strenuous activity for 24 hours. Caregivers should monitor responsiveness, hydration, and wound sites and contact the dental team if concerning symptoms arise. A brief timeline—immediate (0–2 hours), short-term (24 hours), and near-term (72 hours)—helps set realistic expectations for recovery.
Attract new patients and retain existing ones by providing comprehensive information, building trust, and facilitating appointment bookings.
What Are the Most Common Questions About Sedation and Anesthesia in Dentistry?
Patients frequently ask whether sedation is safe and who is eligible; concise, authoritative answers can guide decisions and prepare patients for conversations with their dental teams. Short Q&A responses optimize clarity and help capture direct-answer search intent for common patient queries. The next subsections provide succinct, evidence-informed answers to two of the most frequent concerns: general safety and intravenous moderate sedation.
Is Dental Sedation Safe for All Patients?
Dental sedation is generally safe when individualized to the patient and administered by appropriately trained clinicians using established monitoring protocols; however, not every patient is a candidate for every sedation level, and certain medical conditions or medication interactions require modified approaches or alternative plans. Safety depends on thorough preoperative screening, adherence to fasting and medication guidance, appropriate monitoring devices, and staff trained in airway and emergency management. Patients with complex medical histories may require consultation with their physician or an anesthesiologist to optimize safety. Open communication about health history and current medications is essential to reduce risk.
What Is Intravenous Moderate Sedation and How Does It Benefit Dental Patients?
Intravenous moderate sedation is a controlled sedation technique where sedative medications are administered directly into the bloodstream to achieve a state of relaxation and reduced anxiety while maintaining patient responsiveness and protective reflexes. This method allows precise control over sedation depth, rapid onset, and quick recovery, making it ideal for patients with significant dental anxiety or those undergoing longer or more complex procedures. IV moderate sedation improves patient comfort, reduces procedural stress, and facilitates efficient dental care. It requires continuous monitoring by trained clinicians to ensure safety and effective airway management throughout the procedure.
- If you are considering sedation: Ask your dental team about options, monitoring, and recovery expectations.
- Prepare for your visit: Follow pre-appointment instructions and arrange a responsible escort if required.
- Discuss medical history: Provide a complete medication list and disclose respiratory or other relevant health issues.
Attract new patients and retain existing ones by providing comprehensive information, building trust, and facilitating appointment bookings. To take next steps, request a pre-operative consultation with your dental team to review options, discuss individualized risks and benefits, and schedule any necessary pre-sedation assessments or clearance.
This article covered definitions, types, candidate criteria, benefits, safety protocols, preparation checklists, and common patient questions to help you make informed decisions and feel confident discussing sedation and anesthesia for dental care.